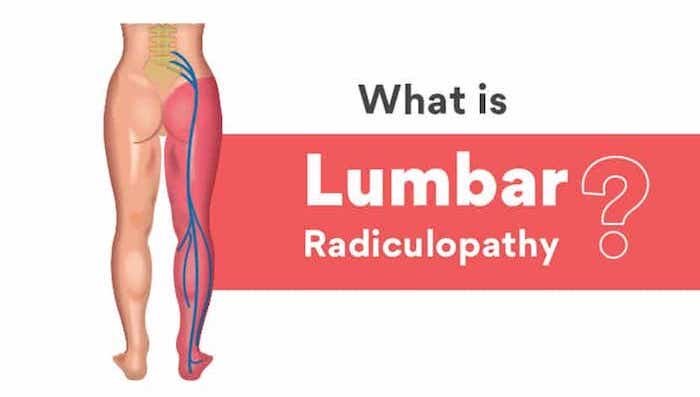
A Low Back Problem Where Irritation of A Spinal Nerve Creates Low Backaches And Leg Pain, Numbness, Or Weakness
Facts and Information About Lumbar Radiculopathy
Lumbosacral radiculopathy is a term that describes an irritated spinal nerve in the low back area. Spinal nerves are large nerves that leave the spine to reach the rest of the body, where they control body movements and a person’s ability to feel pain.
The low back, also known as the lumbar spine, is an area that is likely to suffer injuries and wear and tear. Damage in the lumbar spine may create pressure on a spinal nerve, “pinching” it or create inflammation that causes the nerve to swell.
Since spinal nerves branch off from the low back to reach the legs, a person with a pinched nerve in this area will have low back pain and shooting leg pains, tingling, numbness, or weakness.
Some interesting facts:
- Lumbar radiculopathy can appear at any age but usually affects people between the ages of 30 and 50.
- In a working population where roughly 12.9% of people have low back pain, 11% develop lumbar radiculopathy.
- Lumbar radiculopathy can occur at several different levels in the spine. The exact level determines where a person feels pain in the leg.
How Lumbar Radiculopathy Starts
Lumbar radiculopathy starts when a spinal nerve in the low back is irritated.
A spinal nerve becomes irritated when:
- There is pressure on the spinal nerves as they leave the spine through tiny openings in the backbones. Wear-and-tear, traumas, or arthritis can damage the discs and joints in the spine. Eventually, bone spurs start to grow on the backbones. These changes create a narrowing of the tiny openings through which spinal nerves travel, putting pressure on the nerves and irritating them.
- There is a herniated disc. A herniated disc, also known as a “ruptured” or “slipped” disc, occurs when one of the rubbery pieces of cartilage that sit between the backbones breaks or slips out of place. If the herniated disc presses into a nearby spinal nerve, the “pinched” nerve becomes irritated. A herniated disc may also cause local inflammation and swelling in a spinal nerve without touching the nerve.
Symptoms of Lumbar Radiculopathy
Radiculopathy (a pinched nerve) can appear at all levels of the spine but is most likely to start in high-strain areas like the neck and low back.
The exact place in the spine where radiculopathy occurs determines the body area where a person has pain.
For example:
A pinched nerve in the neck (cervical radiculopathy) causes pain, tingling, numbness, weakness in the shoulder, arm, hand, or fingers.
A pinched nerve is in the mid-back (thoracic radiculopathy) causes chest and torso pain, tingling, and numbness.
A pinched nerve is in the low back (lumbar radiculopathy) may trigger any of the following symptoms:
- Shooting leg pain
- Numbness in a band pattern
- Leg weakness
- A loss of leg reflexes
- Tingling sensations
- Low back pain (in some people)
- Leg paralysis (in severe cases)
- Hip pain and sciatica
- Incontinence/sexual dysfunction (in severe cases)
Diagnosing Lumbar Radiculopathy
A pinched nerve is a common complaint in people who visit a pain specialist. To find the exact place in the spine where you have a pinched nerve, your pain specialist will:
- Obtain a medical history
- Examine the back, check for leg numbness, decreased reflexes, and gait changes
The following tests help:
- X-rays
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Electromyography (EMG)
- Nerve conduction studies
- Selective Nerve Root Injection (SNRI) (helps find the pinched nerve and reduces pain)
Relief for People with Lumbar Radiculopathy
Nerve pain may improve slowly over several days or weeks. A person may need 2-6 weeks of rest, physical therapy, oral medications, and other conservative treatments.
If conservative treatments fail, a pain specialist will provide minimally invasive (non-surgical) treatments that calm the irritated nerve. If a person continues to have pain, the pain specialist will refer them to a surgeon for further evaluation.
Precision Pain Care and Rehabilitation has two convenient locations in Richmond Hill – Queens and New Hyde Park – Long Island. Call the Richmond Hill office at (718) 215-1888, or (516) 419-4480 for the Long Island office, to arrange an appointment with our Interventional Pain Management Specialist, Dr. Jeffrey Chacko.