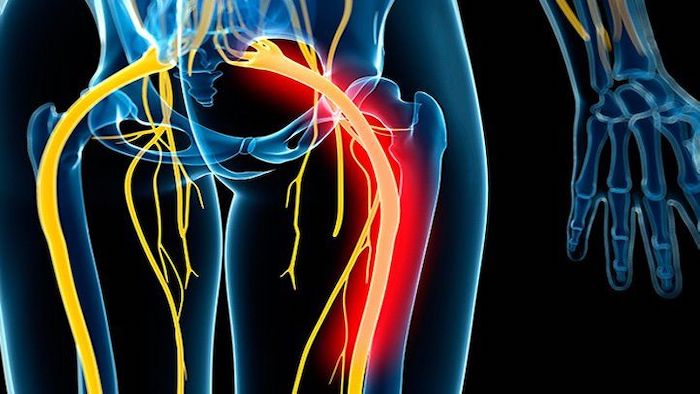
Sciatica is one of the most common complaints of lower back pain. Let’s examine sciatica closer to determine what it is, what causes it, and how to deal with it.
My first experience with sciatica literally brought me to my knees. Working as a paramedic, I stepped out of the back of the ambulance, a motion I had done countless times, and as soon as my foot touched the ground, my leg gave way. Down I went, and the most intense pain I had ever felt seized my back and leg. Sciatica had me firmly in its grip, and it would be months before it let go. Let’s take a closer look at the causes, symptoms, and treatments of this common condition.
What is Sciatica?
Sciatica means pain in the great sciatic nerve that runs from the lower back to the foot. It’s the result of pressure being put on the nerve. The pressure can originate from either misaligned vertebrae or a narrowing in the opening where the sciatic nerve exits the spinal column.
Muscle spasms in the lower back can twist a person’s posture and exert pressure on the sciatic nerve. When sciatica struck me, my back twisted like a pretzel, and I couldn’t stand straight or walk without leaning on something.
The piriformis muscle can also contribute to sciatic pain. This deep muscle runs diagonally through the buttocks from the tailbone to the top of the femur. It helps rotate the leg, and the sciatic nerve runs right underneath it. When this small muscle spasms or becomes inflamed, it irritates the sciatic nerve. Any time a nerve is under pressure or irritated, pain is the result.
What Causes Sciatica?
There are countless ways to trigger sciatica. For some people, simply sneezing or coughing can cause sciatic pain. However, there are some common contributing factors that increase the risk of sciatica.
Spinal problems: Disorders like spinal osteoarthritis, herniated discs, or spinal stenosis (a disorder that causes narrowing of the openings that the nerves exit through leaving the spinal cord) can all result in alignment issues in the back that can directly pinch or put pressure on the sciatic nerve.
Muscle spasms: Back spasms can be incredibly powerful and literally pull a person into a twisted position, which can trigger sciatica. Two of the most common causes of muscle spasms are improper lifting and prolonged sitting. Both are occupational hazards for many people.
Obesity: When a person carries a significant amount of extra weight, it alters their posture, which can then trigger pressure on the sciatic nerve. Obesity also can limit the range of motion in the spine which causes the joints to become stiff. Stiff joints become easily inflamed and that inflammation can cause sciatica flare-up.
What Are the Symptoms of Sciatica?
The primary symptom of sciatica is, of course, pain. The pain typically starts in the low back and often runs down the buttock and leg. It’s usually sharp in nature but sometimes it’s described as burning. Sciatica can also cause numbness in the foot and weakness in the leg. It’s important to note that sciatica generally only affects one side of the body. Sciatic pain can come and go, or it can be constant.
What Is the Treatment for Sciatica?
Treatment for sciatica focuses on pain control and identifying the cause. Once the symptoms are brought under control, then the focus shifts to preventing a flare-up.
Medications: Pain medications like Tylenol, Tramadol, or hydrocodone/oxycodone can be used to temporarily control sciatic pain. They are usually prescribed along with anti-inflammatory drugs like Naproxen or Celebrex. Anti-inflammatory medication is important to decrease the pressure on the sciatic nerve. Steroids like prednisone are also sometimes used for the same purpose.
Ice/Heat: Another standard treatment is ice and heat rotation to the affected area. The ice numbs the area and helps combat inflammation. Ice is always my go-to when my back acts up. Heat soothes tight muscles. Never apply ice or heat sources directly to the skin, and always use a washcloth or towel to protect the skin.
Muscle rubs and pain patches: Muscle rubs and pain patches often contain lidocaine or other numbing agents that are absorbed through the skin. The medication helps numb an area and decreases pain.
Massage: When an area is in pain, we have a tendency not to move it. This contributes to an increase in stiffness and inflammation in the area. Massage can help relax the muscles and stimulate blood flow to the area to combat inflammation and stiffness.
Nerve block: In cases where other methods have failed, doctors will sometimes directly block the sciatic nerve. This requires medication to be injected directly into the nerve where it exits the spinal column. It can offer long-term pain relief without requiring surgery.
Identify the cause:
If spinal issues are suspected, the doctor will usually start with an x-ray and move on to an MRI if necessary. These images determine if the vertebrae are lined up and if there is any narrowing of the passages out of the spinal column. If actual bone issues are the cause of chronic sciatica, surgery is sometimes needed.
How to Prevent Flare-Ups?
Like most disorders, preventing the issue is much preferable to trying to treat it. Here are some of the best ways to avoid a sciatica flare-up.
Sit up straight: Let’s face it. A lot of us sit way more than we ought to. Using proper posture is vitally important to avoid triggering a sciatica flare. First, make sure you’re sitting in a well-supported chair. Adjust it so your feet are squarely on the floor, and your hips and knees are at 90-degree angles. Distribute your weight evenly on both hip bones and sit up straight, putting your shoulders over your hips- no slouching!
Also, be sure whatever you are looking at (computer screen, book, whatever…) is at eye level. If it is in your lap, you’re automatically dropping your chin and moving away from good posture. Lumbar supports can help to accentuate the curve in your back, which helps prevent sciatic pinching.
Get up and move: Long periods of sitting are a common cause of sciatic pain. If you are tied to a desk for most of the day, be sure you take frequent stretch breaks. You can also check out the sit-to-stand desks so you can stand to do your work instead of sitting all the time. Consider setting a timer or using an app to remind you to get up and walk and stretch regularly. Walking and gentle stretching are your best defenses to prevent sciatica. Our pain relief app offers support to incorporate exercise into your daily routine, as well as
Stretching suggestions: You should always double-check with your doctor before implementing any kind of exercise routine. I have a regular set of yoga stretches that keeps my lower back healthy and sciatica at bay. The most important part is to concentrate on stretches that strengthen and stretch your back.
Stretches that target the glutes and hamstrings and improve overall core strength are also integral. You don’t have amazingly flexible or in shape to try these stretches! Just be gentle and don’t go any further than is comfortable.
Precision Pain Care and Rehabilitation has two convenient locations in Richmond Hill – Queens and New Hyde Park – Long Island. Call the Queens office at (718) 215-1888, or (516) 419-4480 for the Long Island office, to arrange an appointment with our Interventional Pain Management Specialist, Dr. Jeffrey Chacko.