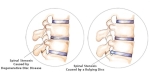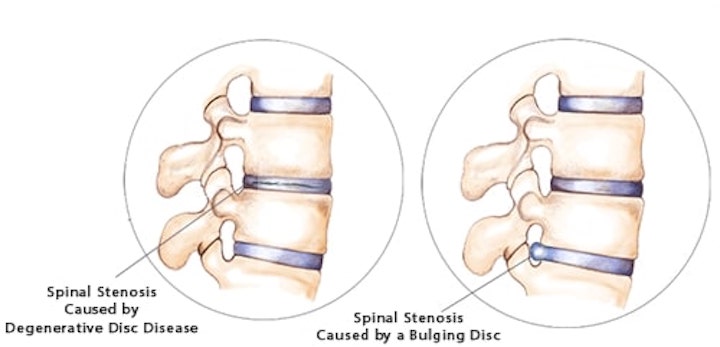
There are a number of potential symptoms of spinal stenosis, and one's specific symptoms are mainly determined by the location and severity of the stenosis in the spine.
Common Spinal Stenosis Symptoms
- Overall, spinal stenosis symptoms are often characterized as:
- Developing slowly over time, or slow onset
- Coming and going, as opposed to continuous pain
- Occurring during certain activities (such as walking for lumbar stenosis, or biking while holding the head upright) and/or positions (such as standing upright for lumbar stenosis)
- Feeling relieved by rest (sitting or lying down) and/or any flexed forward position.
Lumbar Stenosis Symptoms
When stenosis has developed in the lower back (lumbar spine), leg pain with walking may develop.
Leg pain with walking is medically known as claudication, and it can be caused by either arterial circulatory insufficiency (vascular claudication) or from spinal stenosis (neurogenic or pseudo-claudication). Leg pain from either condition will go away with rest, but with spinal stenosis, the patient usually has to sit down for a few minutes to ease the leg and often low back pain, whereas leg pain from vascular claudication will go away if the patient simply stops walking.
For lumbar stenosis, flexing forward or sitting will open up the spinal canal by stretching the ligamentum flavum and will relieve the leg pain and other symptoms, but the symptoms will recur if the patient gets back into an upright posture. Numbness and tingling can accompany the pain, but a true weakness is a rare symptom of spinal stenosis.
Spinal Stenosis Diagnosis
Diagnostic imaging studies for patients with any type of spinal stenosis include either an MRI scan or a CT scan with myelogram (using an X-ray dye in the spinal sac fluid), and sometimes both. Plain CT scans can better identify bony causes of spinal stenosis, but cannot give the same detail for soft tissue causes of stenosis such as disc bulges, disc herniation’s, and ligament hypertrophy. Due to this changing compression, spinal stenosis symptoms vary from time to time and the physical examination generally will not show any neurological deficits or motor weakness. Certain activities and body position may trigger the symptoms.
In some medical centers, upright MRIs, flexion-extension MRIs, and spine load-bearing MRIs have been used to identify the dynamic changes on the spine, and the canal dimensions. The efficacies of these tests are still being studied, but there may be additional information provided by such tests.
Cervical foraminal stenosis can be pinpointed not only by the CT and MRI scans but also by injecting the suspicious nerve with a small volume of local anesthetic. This procedure is called a selective nerve root block.
After the injection, a remission of the patient's symptoms along with true temporary weakness of the limb is clinically diagnostic and can help the surgeon determine the source of symptoms, and potentially reduce the size and complexity of the surgery.
Rarely, a surgeon will use electrodiagnostic studies to determine the type of surgery. Those studies can be helpful in trying to determine if a symptom is caused by neuropathy, rather than radiculopathy. But few surgeons are confident of the specificity provided by these studies. The results will not help plan a surgical procedure but may help decide to cancel one for example if it is a global neuropathic problem, surgery may not be beneficial.
If you are suffering from pain, please contact our office at (516) 419-4480 or (718) 215-1888 to arrange an appointment with our Interventional Pain Management Specialist, Dr. Jeffrey Chacko.