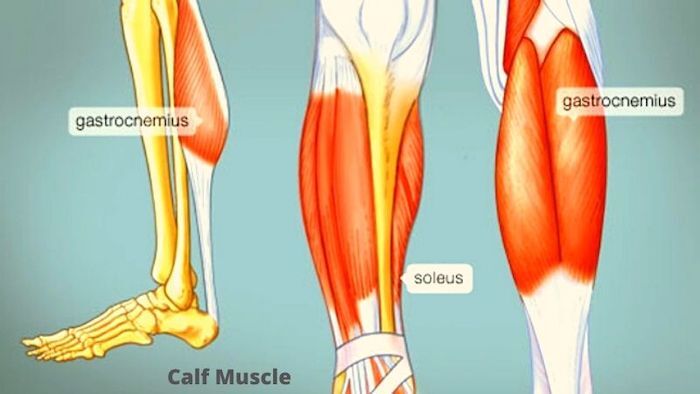
What Are Calf Muscles?
There's a group of muscles on the back of each lower leg that doctors call "calf muscles." They play a key role in helping you walk and run. Lots of things can make them hurt, from a minor sprain to more serious problems like deep vein thrombosis
Muscle Cramp
If you work your calf muscle too much, you can get a sudden pain in your leg. A muscle cramp can also happen if you hold a position too long or haven't had enough water to drink. Most cramps are harmless and improve if you massage yourself, do gentle stretching, and apply a warm towel or heating pad. If it doesn't get better, call your doctor. Although rare, muscle cramps can be caused by other health issues, like compressed nerves.
Muscle Strain
Stretch too far or put too much pressure on your calf, and you can strain your muscle. If so, you'll have a dull ache that worsens when you move. Swelling, redness, or a bruise are also common, and it may hurt to rise up on your toes. Rest and ice can help. When you sit, try to raise your calf higher than hip height. You'll also need to be patient. A pulled muscle can take up to 6 weeks to completely heal.
Achilles Tendinitis
Your Achilles tendon connects your calf muscle to your heel bone. If it gets injured, you'll feel an ache in the back of your leg that's worse after you're active. Your calf could also feel stiff and sore in the morning. Achilles tendinitis often improves with a treatment called RICE (rest, ice, compression, and elevation). If not, your doctor may suggest physical therapy.
Baker's Cyst
The fluid inside your knee helps it move smoothly, but an injury or arthritis can cause too much to build up in the back of your knee. If you have a Baker's cyst, you'll notice swelling and may not be able to straighten your knee. Swelling and redness can also spread to your calf. Sometimes, a Baker's cyst goes away on its own. If not, your doctor may need to look for and treat, the condition causing it.
Sciatica
If the sciatic nerve in your lower back gets pinched or inflamed, you'll feel a burning pain down one, or both, of your legs. Sciatica pain can come and go. It may also get worse after you stand or sit for a while. Ice packs, applied 20 minutes at a time, can help, as can over-the-counter pain medicine. You may also try massage, acupuncture, or yoga. If you still hurt, your doctor may suggest a steroid shot.
Chronic Compartment Syndrome
Inside your legs are pockets of muscles, nerves, and blood vessels. Excessive activity, like too much running, can cause bleeding or swelling inside them. If you have chronic compartment syndrome, a pressure buildup inside your muscles causes your blood flow to go down. Your calf may cramp or hurt when you move. You may see swelling or a muscle bulge. A break from the activity can help. In severe cases, you might need surgery.
Varicose Veins
If you stand or walk a lot, the pressure on your legs can cause varicose veins in one or both calves. These thick, bulging veins can cause pain, burning, swelling, and itching. Compression stockings can help. So can movement and exercise, which help pump blood from the calf. You can also prop up your leg when you sit, and try not to sit or stand for too long. Your doctor may also treat it by closing up or shrinking the veins.
Deep Vein Thrombosis (DVT)
Sometimes, a blood clot forms deep inside your leg. If so, your calf may ache and feel warm. The skin may also look red. Obesity can put you at risk for DVT. So can pregnancy, smoking, and sitting for long amounts of time. If a clot in your leg breaks loose, it can travel to your lungs and cause severe issues, so if you notice any of these symptoms, contact your doctor right away.
Claudication
Calf pain can be a sign that your leg muscles aren't getting enough blood. If you have a problem called claudication, your legs will hurt when you're active, and your feet, thighs, hips, and bottom may also ache. Your doctor can run tests to see how well blood flows to your lower limbs. Some types of medicine can help ease symptoms and prevent other problems. Talk to your doctor about getting regular exercise to ease the pain.
Neurogenic Claudication
The most common cause of this problem is spinal stenosis -- a narrowing of spaces in your spine that puts pressure on nerves. You can have pain, tingling, or cramps in your legs, as well as your hips and bottom. It could get worse when you stand or walk but will stop if you sit or lean forward. If you have neurogenic claudication, you may need surgery to ease the pressure on your nerves
Diabetic Peripheral Neuropathy
Up to half of all people with diabetes get nerve damage. Peripheral neuropathy, which is caused by frequent high blood sugar, can bring numbness, pain, weakness, and a burning feeling in your legs. You may feel it in your feet, arms, and hands, too. Since you may start to lose your balance or find it hard to walk, your doctor can prescribe medicine to treat the pain. Physical therapy can improve your strength.
Lower Leg Fracture
Your shinbone (tibia) helps you bear weight in your lower leg. The bone that runs beside it is your fibula. If either breaks or cracks, your calf may be tender, swollen, or bruised. Walking may be painful, and your lower leg may look shorter than it should. Your doctor may set the bones together and put on a cast to keep them in place while they heal.
Bone Infection
Although it's not common, germs sometimes get into your bones and cause an infection, known as osteomyelitis. When the infection is in a lower leg bone, you'll notice redness, swelling, and warmth in your calf. You may also have a fever and fatigue. If lab and imaging tests confirm that you have a bone infection, you may need antibiotics to remove part of the infected bone.
Precision Pain Care and Rehabilitation has two convenient locations in Richmond Hill – Queens and New Hyde Park – Long Island. Call the Richmond Hill office at (718) 215-1888, or (516) 419-4480 for the Long Island office, to arrange an appointment with our Interventional Pain Management Specialist, Dr. Jeffrey Chacko.