Home »
Blog » Back Pain
| Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
Back Pain | Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
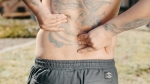
Tags: Back Pain | Posted on: 26-Jun-2024 | No of views: 5433 Lower right back pain is commonly caused by damage or injury to the spinal structures, such as the lower right back muscles, the lumbar intervertebral discs, or the facet joints. While problems with these structures are more likely to cause centralized pain around the spine, pain may be felt primarily or entirely on one side of the spine.
Read more
Tags: Back Pain | Posted on: 24-Jun-2024 | No of views: 5244 Low back pain is sometimes felt entirely or primarily on the right side rather than spread evenly across the back. Understanding the possible causes of lower right back pain and its typical characteristics can help lead to an accurate diagnosis and more effective treatment. General Causes of Lower Right Back Pain: Lower right back pain most commonly results from the following general sources...
Read more
Tags: Back Pain | Posted on: 19-Jun-2024 | No of views: 5975 Muscles in the lower back, abdomen, buttocks, and hips are all necessary for supporting and stabilizing the spine. Keeping these muscles active and strong can help avoid low back injury and minimize pain if the spine becomes injured. A complete back exercise program consists of stretching and strengthening the lower back, abdominal, and lower body muscles, and also includes regular aerobic conditioning.
Read more
Tags: Back Pain | Posted on: 17-Jun-2024 | No of views: 5824 Treatment for low back muscle strain is typically simple and only needed for a short time. A long-term exercise program, or ergonomic or sports modifications, may also be recommended. Aggressive chiropractic manipulation should be avoided at the onset of treatment. It is best to restore health gradually and diligently, watching for worsening symptoms versus improvement.
Read more
Tags: Back Pain | Posted on: 14-Jun-2024 | No of views: 5989 Muscle strain can happen suddenly because of an injury or develop over time due to overuse and repetitive motions. A one-time injury that damages a muscle, tendon, or ligament is an acute muscle strain. These injuries usually occur after sudden, jarring impacts or during activities that include heavy lifting or excess pressure on the spine.
Read more
Tags: Back Pain | Posted on: 12-Jun-2024 | No of views: 6104 The pain from a pulled-back muscle can range from merely irritating to intense and debilitating. Most cases of low back muscle strain start to abate within a couple of hours or days and do not lead to long-term problems. If pain has continued for more than a week or two, or if it is severe enough to disrupt daily activities, seeking medical attention is warranted.
Read more
Tags: Back Pain | Posted on: 10-Jun-2024 | No of views: 5808 Most episodes of low back pain are caused by damage to the soft tissues supporting the lower spine, including muscles, tendons, and ligaments. The lower spine also called the lumbar spine, depends on these soft tissues to help hold the body upright and support weight from the upper body. If put under too much stress, the lower back muscles| or soft tissues can become injured and painful.
Read more
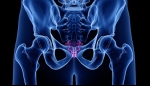
Tags: Back Pain | Posted on: 27-May-2024 | No of views: 7695 Coccydynia is typically diagnosed by gathering a thorough medical history and completing a physical exam. These two standard diagnostic practices are usually sufficient in obtaining a diagnosis and evaluating treatment options, but in some cases, diagnostic tests such as scans or injections may be used.
Read more
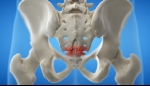
Tags: Back Pain | Posted on: 24-May-2024 | No of views: 8398 Direct trauma to the tailbone is the most common cause of coccydynia and usually leads to inflammation surrounding the coccyx, which contributes to pain and discomfort. There are many cases reported in which pain begins with no identifiable origin (called idiopathic coccydynia).
Read more
Tags: Back Pain | Posted on: 22-May-2024 | No of views: 5844 Tailbone pain is usually accompanied by other, more specific symptoms that can sometimes indicate how pain is occurring. Common Symptoms of Coccydynia - Coccydynia may be further characterized by one or a combination of the following symptoms: Localized pain and tenderness - Pain is generally confined to the tailbone, and does not radiate through the pelvis...
Read more
Love this Post? Spread the World