Most people take the action of walking for granted and don’t realize that they might not be walking correctly.
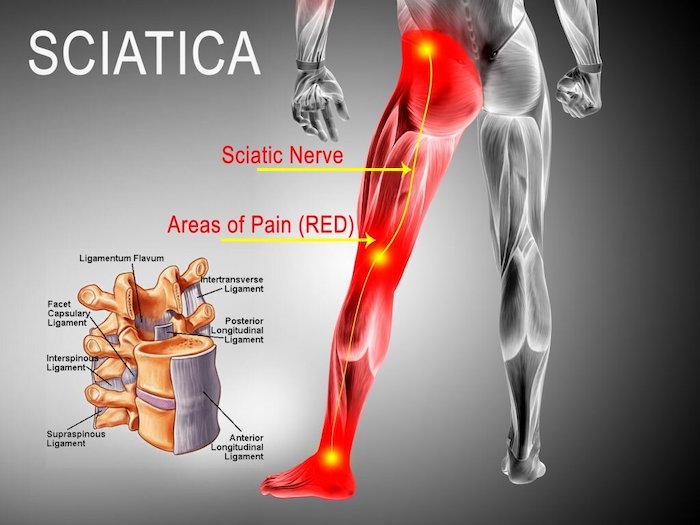
Sciatica occurs because a causative factor, such as a bone, disc, or muscle in your lower back impinges on your sciatic nerve roots. When you walk and stand correctly, you align your bones in a more effective way, creating a better pathway for the course of your sciatic nerve.
Walking Patterns That May Affect Your Sciatic Nerve
The way you walk and stand can affect the path of your sciatic nerve from your lower back to your foot. Incorrect walking patterns can cause misalignment, fatigue, and/or excessive stress on your lower back tissues, which can irritate or compress your sciatic nerve roots, causing sciatica.
The following walking patterns can increase stresses on the joints of your spine, alter your muscle activity, and/or increase the loads on your joints and discs, which may affect your sciatic nerve roots1:
- Walking by excessively curving your lower back. A walking posture that involves thrusting your abdomen and increasing the curve in your lower back (lordotic posture) can cause your spinal facet joints to get overloaded. Also, the muscles that work to support your spine, such as your hip and buttock muscles become underactive and weak, in turn causing your thigh muscles to become overactive to compensate for spinal stabilization.
- Walking with a hunched back. Bending your upper back while walking (kyphotic posture) can cause your chest to tilt forward, increasing the stress within your abdominal and core muscles.
- Walking with a flat back. Walking by reducing the natural curve of your upper and lower spine increases the stresses on the vertebrae of your lower back. Your lower back, hip, buttock, and thigh muscles may become fatigued and/or weak.
- Walking by tipping your pelvis in front. Walking by shifting your upper back backward and your pelvis in front (swayback posture) increases the natural curve of your upper and lower back. This posture can cause your lower back muscles to become tense and hyperactive, leading to fatigue.
Frequently engaging in these walking patterns can make your back muscles weak and over time, lead to lower back problems, such as the growth of bone spurs, causing sciatica. If you have sciatica, these walking patterns can exacerbate your symptoms by increasing your sciatic nerve root irritation or compression.
Tips To Protect Your Sciatic Nerve While Walking
To prevent sciatica or reduce your symptoms while walking, pay attention to your body alignment, the length of your stride, and your walking speed:
- Keep your back in a neutral position with your head positioned on the top of your spine and ears above your shoulders.
- While taking a step, land between your midfoot and heel, then gently roll onto your toes and push off into the next stride. This type of initial foot contact will naturally shorten your strides because it is difficult to roll your foot when it’s far from your body.
- Slow down your pace and take shorter steps. You should be able to comfortably hold a conversation while walking.
It is also important to actively engage your abdominal muscles, breathe rhythmically, and take frequent breaks (if walking long distances) while walking.
If your sciatica flares or worsens when you walk, check your posture and slow down your walking speed. If the symptoms persist, consult a doctor for an accurate diagnostic checkup and treatment plan for your sciatica.
Precision Pain Care and Rehabilitation has two convenient locations in Richmond Hill – Queens and New Hyde Park – Long Island. Call the Richmond Hill office at (718) 215-1888, or (516) 419-4480 for the Long Island office, to arrange an appointment with our Interventional Pain Management Specialist, Dr. Jeffrey Chacko.