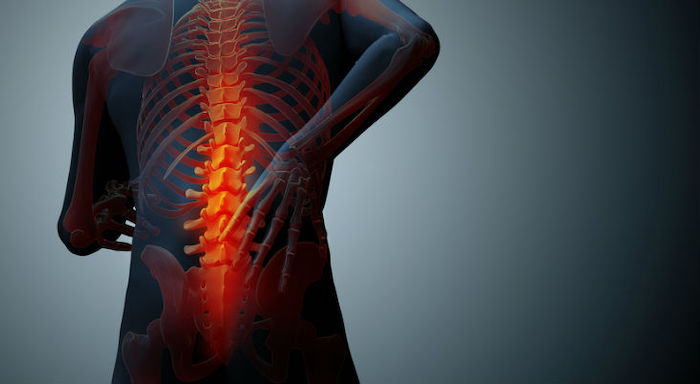
Spinal pain can be debilitating. According to the American Chiropractic Association, it is estimated that 80% of people will experience back pain during their lifetime. The resulting stiffness from back pain can restrict one’s ability to move. Persistent pain may radiate to other parts of the body, including the chest, arms, and legs. As a result, walking properly and maintaining good posture can be difficult. For some patients, it may seem impossible to find a comfortable position since sitting, standing, and even sleeping may prove painful.
PRP Therapy
This revolutionary, natural therapy can be used to treat a variety of concerns including spine pain. Platelet-rich plasma (PRP) is derived from a patient’s own blood. Plasma is the liquid portion of the blood and is mainly composed of proteins and water. It works to circulate red and white blood cells as well as platelets throughout the body. Platelets are the cells responsible for causing the blood to clot. For example, when you get a cut, it is the platelets that work to halt the bleeding. Platelets also contain proteins called growth factors, which promote tissue repair and allow the body to heal itself.
Adults who experience chronic back pain and stiffness may be good candidates for PRP therapy. A small amount of their blood is drawn. It is spun in a centrifuge to separate the platelets from the blood, thus concentrating the growth factors, A local anesthetic may be used to numb the site before the PRP is injected into a targeted area of the back. It may take several weeks following PRP therapy before its optimal and long-lasting results can be experienced. Some patients report that they saw an improvement in their pain for up to six months or more. Because it relies on a patient’s own blood instead of steroidal medications, it is generally considered safe to repeat PRP therapy treatments several times each year to maintain and extend the pain-relieving results.
Epidural Steroid Injections
Steroidal medication is used to nonsurgical treat pain in the cervical, thoracic, and lumbar areas of the spine. With epidural steroid injections (ESI), a corticosteroid and an anesthetic are injected into the spinal nerve to relieve chronic pain that has proven resistant to other types of treatment. By reducing swelling and inflammation, ESI affords the spine an opportunity to rehabilitate and heal from an injury or other pain-producing conditions including a herniated or degenerative disc, spinal stenosis, sciatica, or spondylolysis (also known as a stress fracture).
ESI injections are performed after patients are placed under general anesthesia. A board-certified pain management specialist uses x-ray technology to guide the needle into the epidural space toward the nerve root that is inflamed. One side of the vertebra is treated at a time. Once the needle is in position, the steroid medication is injected.
Following the procedure, it is not unusual for patients to experience some tenderness and discomfort at the injection site. This can be alleviated with over-the-counter medications. Pain relief following an ESI injection may not be instantaneous, so patients should take note of when they notice an improvement in their symptoms. In some cases, additional injections may be necessary in order to experience optimal results.
Spinal Cord Stimulation
Electric pulses are employed as part of spinal cord stimulation therapy to camouflage and ultimately reduce nerve signals that cause chronic pain before they are identified and processed by the brain. This may effectively reduce a patient’s back pain, especially when it has not previously responded well to other forms of treatment. While chronic pain is often the result of sustaining an injury, it also may be due to conditions including arthritis, multiple sclerosis, and nervous system diseases.
Performed as an outpatient procedure, spinal cord stimulation patients are placed under general or local anesthesia before a board-certified pain management specialist inserts a hollow needle into the area between the bone and the spinal cord. The electrical wires of a trial spinal stimulator (SCS) device are placed. The SCS delivers mild electrical currents created by a pulse generator to nerve fibers in the spinal cord. By stimulating nerves in the area where pain has been experienced, the electrical pulses mask the nerve signals before they reach the brain. Patients are released and required to monitor their pain levels. If an improvement is experienced, a permanent device may be placed later beneath the skin. This will allow for better control over the electric pulses and help to secure long-lasting pain relief.
Vertebroplasty
Compression fractures of the spine are often caused by an injury or brittle bone disease known as osteoporosis. These fractures, which can be extremely painful and result in a loss of mobility, may be treated nonsurgically with vertebroplasty. During this minimally invasive procedure, acrylic bone cement is injected into the fracture, causing it to become more stable and for the pain to be alleviated.
Patients are placed under local or general anesthesia to begin their outpatient vertebroplasty procedure. Using an x-ray monitor, a board-certified pain management specialist guides a needle into the fractured vertebra before carefully injecting the bone cement. More than one injection may be required to fill and stabilize the space. Patients must rest on their backs for an hour following the procedure in order to allow the cement to solidify. Most experience pain relief within 48 hours of the procedure.
Precision Pain Care and Rehabilitation has two convenient locations in Richmond Hill – Queens and New Hyde Park – Long Island. Call the Richmond Hill office at (718) 215-1888, or (516) 419-4480 for the Long Island office, to arrange an appointment with our Interventional Pain Management Specialist, Dr. Jeffrey Chacko.