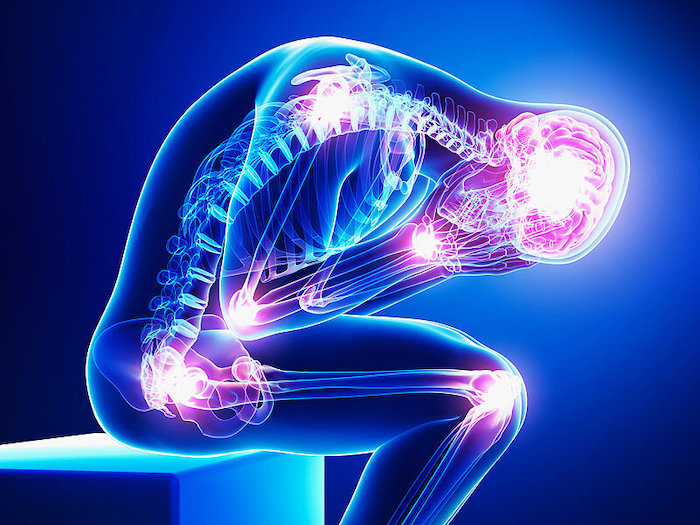
Abnormal Pain That Extends Beyond the Expected Period of Healing
Chronic pain is an enormous problem in the United States, costing millions in lost workdays and decreased efficiency. Chronic pain causes local or widespread pain that remains long after a person recovers from an illness or injury. Unlike short-term pain, chronic pain is abnormal and is considered a disease in itself. If you are one of 100 million Americans who suffer from chronic pain, a pain specialist can treat your pain and help you regain control over your life.
Facts and Information About Chronic Pain
While mostly everyone experiences acute pain, not everyone has chronic pain. Acute pain is the temporary pain experienced after an injury, illness, or surgery. It improves within 1-3 months, as the body heals. Pain that lasts from 3-6 months represents a gray zone where a person may improve or get worse. Pain that extends beyond six months is likely to intensify and become chronic.
Chronic pain may be due to:
- Ongoing illnesses that cause pain, such as cancer or arthritis
- Acute pain that goes untreated
- Damage to sensitive nerves either in the extremities (arms/legs) or in the spine
- Ongoing imbalance in the muscles or joints
- Continued stress on an injured area
- A problem that has not been identified or treated
- Without reason - there is no clear explanation of why some people develop chronic pain, while others remain pain-free
Chronic pain can result from:
- Osteoarthritis
- Rheumatoid arthritis
- Back pain
- Abdominal pain
- Fibromyalgia and myofascial pain
- Inflammatory bowel disease.
- Autoimmune or autoinflammatory disorders (such as multiple sclerosis)
- Trauma
- Prior surgery, especially spine surgery
- Neurological disorders
- Ehlers-Danlos Syndrome
- Headaches
- Cancer
- Complex Regional Pain Syndrome (CRPS)
What Leads to Chronic Pain?
Changes in how a person perceives pain
It is normal for the pain signaling system in the body to be in the “off” setting. Normally, for example, a person’s thumb does NOT throb, ache, or feel tingly. But, when that person accidentally hits the thumb with a hammer, then there is an injury and the pain signaling pathways turn “on”, warning of tissue damage. In most cases, when the thumb injury recovers over a few days or weeks, the pain signaling calms down and goes away, turning back to the “off” position.
However, in a person with chronic pain, there is often a change in how nerves in the arms, legs, lower back, face, etc., communicate with the brain and spinal cord. The pain systems in the body (networks of nerves) get turned “on” and won’t turn “off”.
In people with chronic pain, the pain-sensing (peripheral) neurons start to send excessive pain signals to the spinal cord and brain, causing the nervous system to become overly sensitive and excitable. The end results in our example are that even though the thumb recovers from being hit by the hammer, the person still feels the same or even worse pain for many months or even years after the injury.
Inflammation
Many patients have chronic pain due to ongoing inflammation in the body. Inflammation in the body can result from tissue damage, infection, or an autoimmune process (where the body’s immune system gets confused and starts to attack its own joints, muscles, or nerves). Rheumatoid arthritis is an example of this. Inflammation leads to swelling, soreness, and irritation in the area, and can result in chronic pain.
Musculoskeletal pain
The body is an amazing system of muscles, joints, bones, and nerves that work together to produce sensation, movement, and balance. Changes or imbalances to this system, known as the musculoskeletal system, can lead to injury and chronic pain. Some people are born with these variations. For example, people who inherit Ehlers-Danlos Syndrome have loose, unstable joints and suffer from early-onset osteoarthritis. Other people acquire musculoskeletal issues through trauma, car accidents, surgeries, or wear and tear. Because the body is a finely tuned machine, a problem in one area can lead to changes in other areas.
Other issues related to chronic pain
Chronic pain can often affect the autonomic nervous system, the nerves that control automatic body functions like vessel dilation, sweating, and body temperature. These systems can be altered and lead to ongoing issues like swelling and temperature sensitivity. Also, these nerves that ordinarily do not transmit pain signals can be hijacked and start to transmit and amplify pain signals. An example is CRPS.
Signs and Symptoms of Chronic Pain
People with chronic pain have unique symptoms, such as:
- Pain triggered by an event that usually does not cause pain (allodynia). A mere cold draft can trigger attacks in a person who suffers from migraines.
- An unpleasant sensation that starts suddenly, with or without cause (dysesthesia). A person may experience unusual burning, wetness, or electric shocks in the mouth, scalp, skin, or legs. Common in multiple sclerosis.
- A sharp increase in pain levels after a painful event (hyperalgesia). People treated with opioids for extended periods may develop an exaggerated response to pain.
- Abnormal tingling, burning, or numbness (paresthesia). Long-term diabetics who suffered nerve damage have paresthesia in their hands and feet.
- Depression, fatigue, insomnia, anxiety, and other psychological and physical changes known as Chronic Pain Syndrome. To read more, click here.
Diagnosis for Chronic Pain
Your pain physician will do a careful evaluation of the issues that are causing the pain. A detailed history and a thorough physical examination are necessary and can determine a need for diagnostic tests such as:
- Laboratory tests
- Imaging studies (MRI, CT scans, Ultrasound, X-rays)
- Electromyography
- Nerve conduction studies
Management of Chronic Pain
Conservative treatments include physical therapy, occupational therapy, and chiropractic care. Medications such as anti-inflammatories, nerve medications, muscle relaxants, and antidepressants/anticonvulsants help decrease chronic pain. The next step is treatment with advanced procedures, under the care of a pain specialist.
Precision Pain Care and Rehabilitation has two convenient locations in Richmond Hill – Queens and New Hyde Park – Long Island. Call the Richmond Hill office at (718) 215-1888, or (516) 419-4480 for the Long Island office, to arrange an appointment with our Interventional Pain Management Specialist, Dr. Jeffrey Chacko.