Home »
Blog » Pain Management
| Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
Pain Management | Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
Scoliosis is a condition where the spine curves sideways, often developing during the growth spurt just before puberty. While scoliosis can range from mild to severe, the impact on daily life can be significant, especially when pain becomes a chronic issue. At Precision Pain Care and Rehabilitation, our focus is on helping patients with scoliosis manage their pain effectively through interventional pain management strategies.
Read more
Spinal stenosis is a condition that affects many individuals, particularly as they age. It involves the narrowing of the spinal canal, which can put pressure on the spinal cord and the nerves that travel through the spine. At Precision Pain Care and Rehabilitation, we focus on addressing conditions like spinal stenosis through a combination of interventional pain management techniques that aim to reduce pain and improve function.
Read more
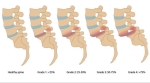
Spondylolisthesis is a spinal condition that can cause significant discomfort and pain, affecting an individual's daily life. Precision Pain Care and Rehabilitation aims to help patients understand their condition and explore effective treatment options to improve their quality of life. Interventional pain management offers targeted and minimally invasive techniques that can bring relief to those suffering from spondylolisthesis.
Read more
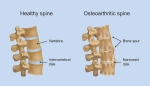
Spinal arthritis, also known as osteoarthritis of the spine, is a common condition that affects millions of Americans, causing pain, stiffness, and decreased mobility. As we age, the cartilage that cushions the joints in our spine can wear down, leading to inflammation, discomfort, and in severe cases, a loss of function. Fortunately, advances in interventional pain management offer targeted relief for those suffering from spinal arthritis.
Read more
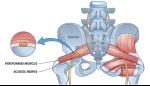
Piriformis Syndrome is often misunderstood and misdiagnosed, yet it is a significant source of pain and discomfort for many people. At Precision Pain Care and Rehabilitation, we focus on providing comprehensive and effective treatment options for conditions like Piriformis Syndrome, emphasizing interventional pain management techniques to improve quality of life.
Read more
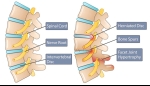
Nerve impingement, medically known as radiculopathy, is a condition that occurs when a nerve in the spine is compressed or irritated, causing pain, weakness, or numbness that radiates to different parts of the body. The pain often extends from the spine to areas such as the shoulders, arms, lower back, or legs, depending on which nerve is affected.
Read more
Muscle spasms are a common and often painful condition in which a muscle involuntarily contracts and tightens. These spasms can occur in various parts of the body and may be triggered by factors like overexertion, dehydration, or muscle strain. At Precision Pain Care and Rehabilitation, Dr. Jeffrey Chacko, MD specializes in interventional pain management, offering targeted treatments for muscle spasms and other musculoskeletal conditions to help patients regain their quality of life.
Read more
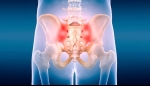
The sacroiliac (SI) joint, located in the lower back where the spine meets the pelvis, plays a critical role in providing stability and absorbing shock during movement. However, when this joint becomes irritated or inflamed, it can lead to a condition known as sacroiliac joint dysfunction (SIJD), causing significant discomfort and impacting one's quality of life.
Read more
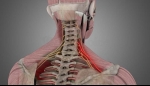
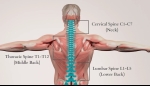
At Precision Pain Care and Rehabilitation, we understand how debilitating a spinal sprain or strain can be. These conditions, which can affect the cervical (neck), thoracic (mid-back), or lumbar (lower back) regions, often lead to significant pain and limit one’s ability to perform daily activities. As an interventional pain management specialist, I, Dr. Jeffery Chacko, MD, am here to provide you with insights into the nature of these injuries, and how interventional pain management can effectively help you find relief and regain mobility.
Read more
Vertebral Compression Fractures (VCFs) are a common yet often under-recognized source of back pain and discomfort, especially in older adults. These fractures can severely impact quality of life, causing pain, reduced mobility, and decreased daily activities. At Precision Pain Care and Rehabilitation, we provide comprehensive care for patients with VCFs,
Read more
Love this Post? Spread the World