Home » Blog
| Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
Blog | Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
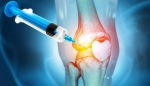
Symptomatic knee osteoarthritis (OA) is a leading cause of disability globally with a significant financial impact. The development of knee OA involves the cartilage and the entire joint, with changes in the articular bone, synovial membrane, joint capsule, ligaments, and musculature around the joint. There is no disease-modifying therapy for the management of OA; therefore, the treatment goals are to improve pain and function.
Read more
Musculoskeletal pain is the most common pain reported by patients. Platelet-rich plasma (PRP) is widely used to treat musculoskeletal pain. However, the efficacy of PRP to treat this pain remains controversial. This review highlights the application of PRP in the treatment of musculoskeletal pain. PRP treatment appears to reduce pain and improve function in patients with musculoskeletal pain.
Read more
More than 20% of adults in the United States suffer from chronic pain, which is persistent pain that lasts three or more months. This pain affects your physical, emotional, social, and financial well-being. Platelet-rich plasma (PRP) therapy is becoming a popular treatment for people suffering from chronic pain. Here, we share five benefits of PRP therapy for chronic pain.
Read more
Platelet-rich plasma consists of two elements: plasma, or the liquid portion of blood, and platelets, a type of blood cell that plays an important role in healing throughout the body. Platelets are well-known for their clotting abilities, but they also contain growth factors that can trigger cell reproduction and stimulate tissue regeneration or healing in the treated area. Platelet-rich plasma is simply blood that contains more platelets than normal.
Read more
Limited evidence exists in current medical literature to support certain whiplash treatment methods over others. Aside from a consensus on staying active (if possible), many treatment options appear to come down to the patient’s unique situation and symptoms, as well as preference. For most people, whiplash results in mild ligament sprains and/or muscle strains that heal within a few days or weeks.
Read more
Whiplash is diagnosed by a clinician when the patient reports some neck pain in the aftermath of trauma capable of causing an acceleration-deceleration injury – most commonly a motor vehicle accident. However, the specifics of a whiplash diagnosis can be complex and have long been the subject of controversy. In the mid-and late-1800s, there were increasingly common disputes regarding train passengers injured in collisions and whether their claims of the mysterious “railway spine” were legitimate.
Read more
For some people, whiplash symptoms can be so minor that they go away within a couple of days. For others, the symptoms can become varied and chronic, ranging from severe pain to cognitive and emotional problems. Whiplash symptoms might manifest immediately following the acceleration-deceleration accident, or they can appear in a few hours or days. Oftentimes the exact underlying cause remains unknown for some whiplash symptoms despite today’s best diagnostic techniques.
Read more
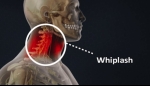
Whiplash occurs when the neck and head are suddenly forced backward and forward, putting the cervical spine through lightning-quick motions and extreme stresses. Most cases of whiplash are caused by car accidents where the person has been rear-ended. Other potential whiplash causes, while comparatively rare, can include assault, bungee jumping, rollercoaster, football, falls while skiing or during equestrian events and other high-impact activities where extreme acceleration-deceleration forces might be applied to the cervical spine.
Read more
The pectoralis major is a powerful chest muscle that causes the arm to move forward, rotate inward, and move closer to the body. The muscle originates from the sternum (breastbone) and the clavicle (collarbone). These two sections of the muscle come together into the pectoralis major tendon, which connects the muscles to the upper arm's humerus bone, near the biceps tendon.
Read more
Persistent or newly developed pain in the lower back after pregnancy, also known as postpartum back pain, usually lasts for 6 months but may continue up to a decade. Postpartum back pain mostly occurs while performing activities that involve body movements, such as walking, lifting, bending, and carrying the new baby, and may be relieved with rest, exercise, and home treatments. The type and severity of pain depend on the underlying cause.
Read more
Love this Post? Spread the World