Home » Blog
| Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
Blog | Stem Cell, PRP, Acupuncture in Queens & Long Island, New York
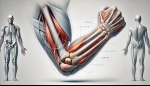
Golfer's elbow, medically known as medial epicondylitis, is a condition characterized by pain and inflammation on the inner side of the elbow. This ailment results from overuse or repetitive stress, leading to microtears in the tendons that attach to the medial epicondyle—the bony prominence on the inside of the elbow. While commonly associated with golfers, this condition can affect anyone engaging in activities that involve repetitive wrist and forearm motions.
Read more
What Are Elbow Sprains and Strains? An elbow sprain involves stretching or tearing the ligaments—the tough bands of tissue connecting bones—within the elbow joint. This typically occurs due to a sudden force, such as a fall onto an outstretched hand or a direct blow to the elbow. Conversely, an elbow strain refers to an injury of the muscles or tendons around the elbow, often resulting from overuse or excessive stretching.
Read more
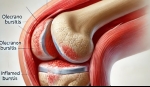
Olecranon bursitis, commonly known as "student's elbow," is an inflammation of the bursa located over the olecranon process at the elbow's tip. This condition can cause pain, swelling, and limited elbow movement, affecting daily activities and quality of life. Interventional pain management offers effective strategies to alleviate symptoms and address the underlying causes of olecranon bursitis.
Read more
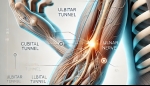
Tags: Arm Pain | Posted on: 25-Dec-2024 | No of views: 5121 Ulnar neuropathy, commonly known as ulnar nerve entrapment, is a condition characterized by the compression or irritation of the ulnar nerve, which runs along the inner side of the elbow down to the hand. This nerve is responsible for the sensation in the fourth and fifth fingers and controls several hand muscles. When compromised, it can lead to symptoms such as numbness, tingling, and weakness in the affected hand.
Read more
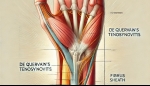
Tags: Arm Pain | Posted on: 23-Dec-2024 | No of views: 5587 De Quervain’s Tenosynovitis is a painful condition affecting the tendons on the thumb side of your wrist. It occurs when the two tendons around the base of the thumb become inflamed, leading to pain and swelling near the thumb and lower arm. This inflammation can cause discomfort when forming a fist, grasping objects, or turning the wrist.
Read more
Tendonitis is a common condition that can cause significant discomfort and disrupt daily activities. It occurs when a tendon—the thick, fibrous cord connecting muscle to bone—becomes inflamed due to overuse, injury, or age-related degeneration. At Precision Pain Care and Rehabilitation, our focus on interventional pain management provides advanced treatment options to help patients find relief and regain mobility. This blog explores tendonitis, its causes, symptoms, treatment options, and how interventional pain management can be an effective approach for long-term recovery.
Read more
Tags: Arm Pain | Posted on: 18-Dec-2024 | No of views: 6094 Ganglion cysts are one of the most common noncancerous lumps that form near the joints or tendons of the body. While they are generally harmless, they can cause pain, discomfort, and functional limitations, especially if they compress surrounding nerves. At Precision Pain Care and Rehabilitation, addressing such conditions with minimally invasive techniques is a cornerstone of effective interventional pain management. Let’s explore the intricacies of ganglion cysts, their symptoms, and the latest treatments available.
Read more
Tags: Arm Pain | Posted on: 16-Dec-2024 | No of views: 4627 Carpal Tunnel Syndrome (CTS) is a prevalent condition that affects millions of Americans annually. This condition, caused by compression of the median nerve as it travels through the carpal tunnel in the wrist, can lead to pain, numbness, and weakness in the hand and wrist. At Precision Pain Care and Rehabilitation, we specialize in comprehensive solutions, including interventional pain management, to help patients regain function and improve their quality of life.
Read more
Arthritis in the hand and wrist is a common condition that can significantly impact daily life, limiting the ability to perform simple tasks such as gripping, writing, or lifting. As the hands and wrists are essential for most activities, arthritis in these areas can lead to pain, stiffness, and reduced functionality. At Precision Pain Care and Rehabilitation, interventional pain management techniques provide effective relief and help restore quality of life for patients.
Read more
Tags: Arm Pain | Posted on: 11-Dec-2024 | No of views: 4385 Wrist and hand injuries, such as sprains and strains, are common among people of all ages. These injuries can occur due to falls, overuse, or direct trauma, affecting everyday activities and professional tasks. At Precision Pain Care and Rehabilitation, the focus is on providing comprehensive and minimally invasive treatments to address such conditions, using interventional pain management techniques to help patients regain functionality and reduce discomfort.
Read more
Love this Post? Spread the World